Can You Switch Your Florida Medicaid Long-Term Care Plan? Here's How.
If you or a loved one is enrolled in Florida’s Long-Term Care (SMMC-LTC) Medicaid program, you are receiving services through a Long-Term Care Managed Care Organization —commonly called an LTC MCO. These are the private health plans that manage home-and-community-based services, nursing facility care, and assisted living facility services for Medicaid recipients in Florida.
While enrollees are generally expected to stay with their chosen plan, Florida law does allow you to switch to a different LTC MCO under certain circumstances. Knowing when and how you can make that change can make a significant difference in the quality of care you or your loved one receives.
This article explains the process for changing LTC MCOs in Florida, who to call, and the approved reasons you may request a plan change outside of open enrollment.
What Is an LTC MCO?
Florida’s Statewide Medicaid Managed Care (SMMC) Long-Term Care program (LTC) is administered by the Agency for Health Care Administration (AHCA) under §409.969, Florida Statutes. Under this program, eligible Medicaid recipients who need nursing facility-level care are enrolled into one of several LTC MCOs operating in their region.
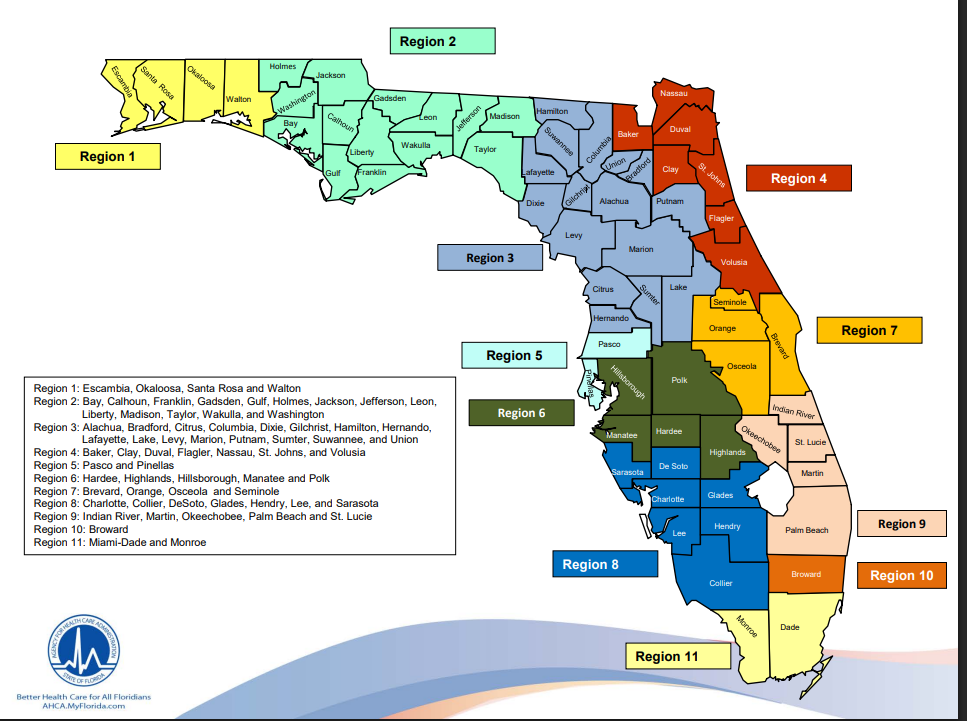
LTC MCOs are responsible for coordinating and covering a wide range of long-term care services, including:
• Nursing facility care
• Assisted living facility (ALF) services
• Home health aide and personal care services
• Adult day health care
• Care coordination and case management
Your LTC MCO plays a central role in determining which providers are available to you, what services are authorized, and how quickly those services are delivered. If your plan is not meeting your needs, you may have the right to switch.
How Do You Change Your LTC MCO in Florida?
The process for changing your LTC MCO in Florida is straightforward — but it must go through the right channel. The way to request a plan change is to contact Choice Counseling, which is the state’s designated enrollment assistance program. Choice Counselors are trained to help Medicaid enrollees understand their options and process plan change requests.
📞 Contact Choice Counseling to Change Your LTC MCO
Phone: 1-877-711-3662
TTY: 1-866-467-4970
Available Monday–Friday, during business hours. Have your Medicaid ID ready when you call. You can also visit the Statewide Medicaid Managed Care Website at the link.
When you call Choice Counseling, you will speak with a trained counselor who will review your request, ask about your reasons for wanting to change, and guide you through the next steps. Depending on the reason for your request, you may need to provide documentation or show that you have already filed a grievance with your current MCO.
It is important to act promptly. Once a change is approved, it typically takes effect at the beginning of the following month. If your current plan is denying or delaying critical services, do not wait; call Choice Counseling and, if appropriate, contact an elder law attorney who can help advocate on your behalf.
When Can You Change Medicaid Plans? Open Enrollment vs. Special Circumstances
Florida Medicaid enrollees generally have the ability to change LTC MCOs during open enrollment periods (90 days from initial enrollment, you can switch for any reason; or 60-days at each anniversary). Outside of open enrollment, however, a plan change requires a qualifying reason. These reasons are defined in Florida Administrative Code Rule 59G-8.600 and § 409.969, Florida Statutes.
Below is an overview of the approved reasons for requesting a plan change outside of open enrollment. Note that many of these categories require you to first file a formal grievance with your current LTC MCO before a plan change will be approved.
1. Access and Network Issues within the Medicaid MCO
One of the most common and straightforward reasons to request a plan change is a problem with provider access. Under Fla. Admin. Code R. 59G-8.600, AHCA recognizes the following access-related grounds:
• Your current nursing facility or assisted living facility has left the plan’s network, and you do not want to change facilities.
• You lack access to medically necessary services or specialists within the plan’s network.
• There are no providers in the network with experience treating your specific medical condition.
In plain terms: if your doctor, nursing home, or ALF is no longer in your plan’s network and you want to keep that provider, that is a recognized basis for a plan change. This is one of the clearer-cut situations, and Choice Counseling generally accepts it when properly documented.
2. Quality of Care and Service Problems
Quality concerns are also recognized basis for a plan change, though these typically require an additional step: you must generally file a formal grievance with your current LTC MCO before AHCA will approve the change. Qualifying quality-of-care reasons include:
• Poor quality of care that does not meet your medical needs.
• Unreasonable delays in the authorization or delivery of services.
If you are experiencing these problems, it is wise to document everything in writing: the dates services were requested, what was denied or delayed, and any communications with your care coordinator. This documentation will support both your grievance and your plan change request.
3. Care Coordination and Clinical Risk
Sometimes the problem is not a single denied service, but an inability to coordinate multiple services simultaneously within the same network. Under Fla. Admin. Code R. 59G-8.600, a plan change may be approved if:
• Needed concurrent services are not all available within the plan’s network, creating a clinical risk to the member.
For example, if a member requires overlapping services — such as specialized wound care and behavioral health support — and the current plan cannot coordinate both, that may qualify as a basis for a plan change on clinical risk grounds.
4. Moral or Religious Objections to a Covered Service
If your current plan covers a service to which you have a sincere moral or religious objection, and you wish to be served by a plan that does not offer that service or offers an alternative, this is recognized as a valid basis for a plan change under Fla. Admin. Code R. 59G-8.600.
5. Fraudulent Enrollment or Forced Provider Changes
Two additional clear-cut reasons for a plan change are recognized under Florida law:
• You were enrolled in the current plan through fraudulent means.
• A change in the plan’s network has forced you to switch providers involuntarily.
In either situation, documentation is key. If your current facility has left the network and you were not properly notified or given adequate time to transition, that strengthens your case for an immediate plan change.
What to Say When You Call Choice Counseling
When you call Choice Counseling to request a plan change, clear and specific language matters. Here are some examples of how to frame your request based on your situation:
• “My current plan does not have providers who can meet my medical needs.”
• “My doctor / nursing facility / ALF is no longer in-network and I do not want to change providers.”
• “I am experiencing delays in getting medically necessary services approved.”
• “The quality of care I am receiving through my current plan is not acceptable.”
Be prepared to explain your situation in detail and to follow up with documentation if the counselor requests it. If you have already filed a grievance with your current MCO, have that information ready as well.
Don’t Skip the Grievance Step; It May Be Required
For several of the qualifying reasons described above - particularly quality-of-care and service delay issues -you may be required to first file a formal grievance with your current LTCMCO before AHCA will approve a plan change. A grievance is a written complaint submitted to the plan notifying them of the problem and requesting resolution.
Filing a grievance serves two purposes: it gives the plan an opportunity to fix the problem, and it creates a documented record that can support your plan change request if the problem is not resolved. Under Florida law, LTC MCOs are required to acknowledge and respond to grievances within specific timeframes.
If you are unsure whether you need to file a grievance first, or if your current MCO is not responding properly to your grievance, an elder law attorney can help you navigate the process.
The Legal Authority Behind These Rights
The right to change LTC MCOs in Florida is grounded in two primary sources of law:
• Section 409.969, Florida Statutes: which governs the Statewide Medicaid Managed Care program and establishes enrollee rights and protections.
• Florida Administrative Code Rule 59G-8.600: which is promulgated by AHCA and provides the specific procedural rules governing enrollment, disenrollment, and plan changes in the LTC program.
These rules are routinely applied by AHCA and Choice Counseling when evaluating plan change requests. When a request is properly documented and supported by one of the qualifying reasons described above, it is generally accepted.
Need Help Navigating Florida Medicaid? We’re Here for You.
Changing your LTC MCO can feel overwhelming, especially when you are already managing the stress of a serious health condition or caring for an aging loved one. Understanding your rights under Florida law, and knowing how to assert them, can make a real difference in the care you receive.
At Elder Needs Law, we help Florida families with Medicaid planning, long-term care planning, special needs planning, estate planning, and probate throughout the state of Florida. If you have questions about your LTC MCO, a denial of services, a grievance, or any aspect of Florida Medicaid, we encourage you to reach out to our firm.
Contact Elder Needs Law today to speak with a Florida elder law attorney who can help protect your rights and your access to care.







